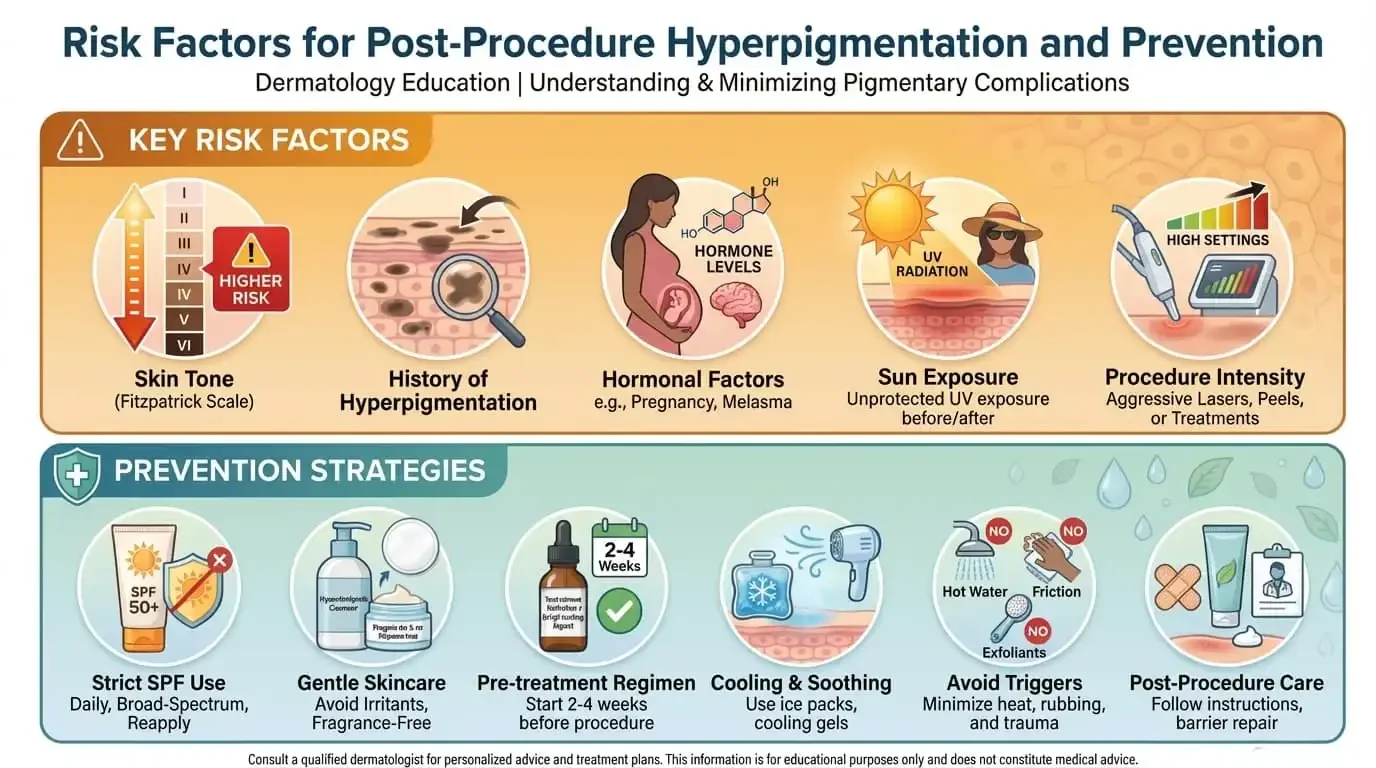
Preventing Hyperpigmentation After Aesthetic Procedures
You invested in an aesthetic procedure to improve your skin, not to trade one concern for another. Yet one of the most common fears patients express before treatment is the possibility of developing dark spots or patches afterward. This concern is valid. Post-inflammatory hyperpigmentation is a real risk following many aesthetic procedures, and once it develops, it can be frustratingly difficult to resolve.
The good news is that hyperpigmentation after aesthetic procedures is largely preventable. Understanding why it occurs, recognizing your personal risk factors, and implementing proven prevention strategies dramatically reduces your chances of developing unwanted pigmentation. The choices you make before, during, and especially after your procedure play a decisive role in whether your skin heals with the beautiful, even tone you envisioned.
Understanding Why Hyperpigmentation Occurs After Procedures
Hyperpigmentation after aesthetic procedures is typically post-inflammatory hyperpigmentation, commonly called PIH. This occurs when inflammation triggers melanocytes, the cells responsible for producing pigment, to go into overdrive. The excess melanin they produce deposits in the skin, creating dark spots or patches that can persist for months or even years.
Aesthetic procedures work by creating controlled injury that stimulates your skin's healing response. This controlled damage is intentional and produces the collagen stimulation, cellular renewal, and skin improvements you are seeking. However, the inflammatory response that accompanies healing can trigger melanocyte activity in susceptible individuals.
The connection between inflammation and pigmentation explains why proper aftercare is so important. Anything that prolongs or intensifies inflammation increases your risk of hyperpigmentation. Conversely, strategies that help your skin move through the inflammatory phase efficiently reduce this risk.
Thermal injury adds another layer of risk. Procedures involving heat, such as laser treatments, IPL, and RF microneedling, can directly stimulate melanocytes. The combination of thermal stimulation and inflammatory response makes these procedures higher risk for pigmentation issues, particularly in predisposed individuals.
Risk Factors for Post-Procedure Hyperpigmentation
Certain factors increase your likelihood of developing hyperpigmentation after aesthetic procedures. Understanding your personal risk profile helps you and your practitioner make informed decisions about treatment selection and aftercare intensity.
Skin Tone
Fitzpatrick skin types III through VI, which include medium to dark skin tones, carry higher risk for post-inflammatory hyperpigmentation. This is because these skin types have more active melanocytes that respond more readily to inflammatory triggers. However, lighter skin types are not immune, particularly with sun exposure during recovery.
History of Hyperpigmentation
If you have experienced PIH previously, whether from acne, injuries, or past procedures, you are more likely to develop it again. A personal history of melasma also indicates increased melanocyte reactivity and higher risk.
Hormonal Factors
Hormonal fluctuations affect melanocyte activity. Pregnancy, oral contraceptives, and hormone replacement therapy can increase susceptibility to hyperpigmentation. If you are experiencing hormonal changes, discuss timing considerations with your practitioner.
Sun Exposure
Recent sun exposure before treatment or any sun exposure during recovery significantly increases hyperpigmentation risk. UV radiation directly stimulates melanin production. When combined with the inflammatory state of healing skin, this creates ideal conditions for pigmentation problems.
Procedure Type and Intensity
More aggressive procedures that create greater inflammation or thermal injury carry higher hyperpigmentation risk. Ablative lasers, deep chemical peels, and intensive treatments require more careful prevention strategies than gentler procedures. For specific aftercare by procedure type, see our guides on laser skin resurfacing aftercare, chemical peel aftercare, and IPL aftercare.
Proven Strategies for Preventing Hyperpigmentation
Implementing these strategies before, during, and after your procedure dramatically reduces your risk of developing unwanted pigmentation.
Pre-Treatment Preparation
Prevention begins before your procedure. If you have higher risk factors, your practitioner may recommend preparatory steps in the weeks leading up to treatment.
Avoid sun exposure for at least two weeks before your procedure, longer if possible. Tanned skin is more reactive and prone to pigmentation issues. If you have unavoidable sun exposure, postpone your treatment.
Some practitioners recommend pre-treatment with ingredients like niacinamide, vitamin C, or practitioner-directed lightening agents to calm melanocyte activity before creating controlled injury. Discuss whether this approach is appropriate for your situation.
Discontinue any photosensitizing medications or products if medically appropriate and approved by your doctor. Certain antibiotics, anti-inflammatory drugs, and skincare ingredients increase sun sensitivity and may affect healing.
Sun Protection During Recovery
This cannot be emphasized enough. Sun exposure during recovery is the single most significant controllable risk factor for post-procedure hyperpigmentation. Your healing skin is exceptionally vulnerable, and even brief UV exposure can trigger pigmentation that may be permanent.
Apply broad-spectrum SPF 50 or higher every single morning throughout recovery. Reapply every two hours if you have any outdoor exposure. Physical sunscreens containing zinc oxide or titanium dioxide are often preferred during recovery as they are less likely to irritate sensitive skin.
Beyond sunscreen, practice active sun avoidance. Stay indoors during peak UV hours of 10am to 4pm when possible. Wear wide-brimmed hats that shade your face completely. Seek shade whenever outdoors. Consider UV-protective window film for your car if you have a long commute.
Continue strict sun protection for at least four to six weeks after your procedure, even after visible healing completes. Newly formed skin remains more susceptible to UV-induced pigmentation for an extended period.
Managing Inflammation Effectively
Since inflammation triggers melanocyte activity, controlling inflammation during recovery directly reduces hyperpigmentation risk. This means using products specifically designed to modulate the inflammatory response without suppressing the healing process.
Plant exosomes derived from Centella Asiatica and Panax Ginseng help regulate inflammation at the cellular level. These microscopic lipid vesicles support intercellular communication, helping your skin cells coordinate healing efficiently without prolonged inflammatory signaling.
PDRN activates tissue regeneration pathways through adenosine A2A receptor signaling while simultaneously reducing the inflammatory response. By shortening the duration of active inflammation, PDRN indirectly reduces the window during which melanocytes are being stimulated.
Niacinamide is particularly valuable for pigmentation prevention. It works by inhibiting melanosome transfer from melanocytes to surrounding keratinocytes, reducing the visible accumulation of pigment even when some melanocyte stimulation occurs. This makes it an essential ingredient in any pigmentation-prevention aftercare strategy.
Avoid anything that increases inflammation during recovery. This includes heat exposure, harsh skincare products, picking at healing skin, and physical irritation. Each inflammatory trigger is an opportunity for melanocytes to activate.
Supporting Efficient Healing
The faster your skin completes the healing process, the shorter the window of vulnerability for hyperpigmentation development. Supporting efficient healing means providing your skin with the ingredients it needs for rapid repair.
NAD+ fuels cellular energy production, enabling your skin cells to perform the intensive work of regeneration efficiently. Adequate cellular energy supports faster progression through healing phases.
Peptides and growth factors signal your skin to produce collagen and rebuild tissue. These ingredients accelerate the repair process, reducing the overall duration of the inflammatory state.
Proper hydration supports all aspects of healing. Dehydrated skin heals more slowly and may experience prolonged inflammation. Keep your skin consistently moisturized throughout recovery.
The most effective approach to pigmentation prevention combines all of these strategies in one cohesive aftercare protocol: inflammation modulation, barrier support, cellular energy, tissue repair signaling, and melanin transfer inhibition working together. This is why multi-technology formulations designed specifically for post-procedure skin outperform single-ingredient products when even-toned healing is the goal.
Avoiding Common Mistakes
Certain behaviors significantly increase hyperpigmentation risk and should be strictly avoided.
Do not pick at healing skin. Picking causes additional injury and inflammation, directly triggering melanocyte activity at those sites.
Do not use active ingredients too soon. Retinoids, acids, and vitamin C can irritate healing skin and prolong inflammation. Wait until your practitioner approves before reintroducing.
Do not skip sun protection on cloudy days or when staying indoors. UV radiation penetrates clouds and windows. Consistent protection is essential.
Do not ignore early signs of pigmentation. If you notice darkening during recovery, intensify your prevention strategies and contact your practitioner for guidance.
What to Do If Hyperpigmentation Develops
Despite best efforts, some patients may still develop pigmentation. Early intervention offers the best outcomes.
Contact your practitioner promptly if you notice darkening that seems abnormal. They can assess whether it is expected healing versus problematic hyperpigmentation and recommend appropriate intervention.
Intensify sun protection immediately. Any additional UV exposure will worsen developing pigmentation.
Continue gentle, anti-inflammatory aftercare. Avoid the temptation to add aggressive brightening treatments while skin is still healing.
Be patient. Post-inflammatory hyperpigmentation often fades over time, particularly with consistent sun protection and appropriate skincare. Some cases may require professional treatment once healing is complete.
Concerned about pigmentation risk with your upcoming or recent procedure?
Frequently Asked Questions
-
Individuals with Fitzpatrick skin types III through VI (medium to dark skin tones) carry the highest risk due to more active melanocytes. However, anyone with a history of hyperpigmentation, melasma, or PIH from past injuries or procedures is also at elevated risk regardless of skin tone. Hormonal factors and recent sun exposure further increase susceptibility.
-
Maintain strict sun protection for at least four to six weeks after your procedure, even after visible healing completes. Newly formed skin remains more vulnerable to UV-induced pigmentation for an extended period. Many practitioners recommend making rigorous sun protection a permanent habit to protect your results long-term.
-
Yes, post-inflammatory hyperpigmentation can often be improved with appropriate treatment. Options include topical brightening agents, chemical peels, and certain laser treatments. However, treatment should only begin once healing from the original procedure is complete. Prevention is always preferable to treatment, as some pigmentation can be stubborn to resolve.
-
Discuss your history and concerns with your practitioner before any procedure. They may recommend less aggressive treatment options, additional pre-treatment preparation, or modified protocols for higher-risk patients. Many procedures can be safely performed on pigmentation-prone skin with appropriate precautions and vigilant aftercare.
-
No, hyperpigmentation can develop days to weeks after a procedure, sometimes after initial healing appears complete. This delayed onset is why continued sun protection and proper aftercare remain important even when your skin looks healed. Monitor your skin throughout the full recovery period and report any concerning changes to your practitioner.
This content is for informational purposes only and does not constitute medical advice. Always follow the specific aftercare instructions provided by your practitioner, as recommendations may vary based on your individual treatment and skin type.