For Practitioners: Optimizing Patient Outcomes with Advanced Aftercare Protocols
The procedure is complete. Your technique was flawless. Yet the outcome your patient ultimately experiences will be determined as much by what happens in the following 14 days as by what happened on your treatment table. Post-procedure care has emerged as the defining variable between good results and exceptional ones, and between satisfied patients who return and refer, and disappointed patients who don't.
For too long, aftercare has been treated as an afterthought in aesthetic medicine: a photocopied handout, a verbal list of don'ts, a hope that patients will figure it out. This approach no longer serves our patients or our practices. The evidence is clear: standardized, evidence-based aftercare protocols directly improve healing times, reduce complications, enhance outcomes, and increase patient satisfaction scores.
This resource is designed for aesthetic practitioners, dermatologists, plastic surgeons, medical spa physicians, nurse practitioners, and aesthetic nurses, who recognize that optimizing the post-procedure phase is both a clinical imperative and a practice differentiator. Here, we'll examine the science of post-procedure recovery, explore protocol design principles, and introduce advanced technologies that can elevate your aftercare offerings.
The Business Case for Standardized Aftercare
Before examining the clinical rationale, let's address the practice management reality: aftercare directly impacts your bottom line, your reputation, and your daily operations.
The Hidden Cost of Inadequate Aftercare
Consider what happens when aftercare is inconsistent or inadequate. Patients experience prolonged redness, unexpected peeling, or anxiety about whether their recovery is normal. They call your office seeking reassurance. Your staff spends time fielding these calls, time that could be spent on revenue-generating activities. Some patients require additional appointments to address complications or concerns. A subset become dissatisfied and share their experience in reviews or word-of-mouth, affecting your reputation and referral pipeline.
Research indicates that patient satisfaction with aesthetic procedures correlates strongly with the post-treatment experience, not just the treatment itself. A study published in Aesthetic Surgery Journal found that patients who feel supported during recovery report significantly higher satisfaction levels, even when experiencing expected side effects like redness or peeling. The perception of care matters as much as the clinical outcome.
The Opportunity in Optimized Aftercare
Practices that implement standardized aftercare protocols report measurable benefits. Reduced callback volume frees staff for higher-value activities. Patients who receive clear guidance experience less anxiety and report higher satisfaction. Optimized healing means patients see results faster, reinforcing their decision to choose your practice. Satisfied patients become referral sources, studies show that positive word-of-mouth remains the primary driver of new patient acquisition in aesthetic medicine.
Additionally, curated aftercare products represent a revenue stream that aligns patient interests with practice economics. Patients want effective recovery products; practices can provide them while generating margin. The key is offering products that genuinely outperform generic alternatives, products that make a visible difference in healing.
Aftercare as Practice Differentiation
In a competitive market, clinical skill alone no longer differentiates practices. Patients expect excellent technique. What distinguishes exceptional practices is the complete patient experience, and aftercare is a significant component of that experience.
Practices known for thorough, supportive post-procedure care develop reputations that attract discerning patients. These patients typically have higher lifetime value, pursue more treatments, and generate more referrals. Investing in aftercare protocols is investing in the patient relationships that sustain practice growth.
The Science of Post-Procedure Recovery
Effective aftercare protocols are grounded in the physiology of wound healing. Understanding these mechanisms enables evidence-based protocol design.
The Wound Healing Cascade
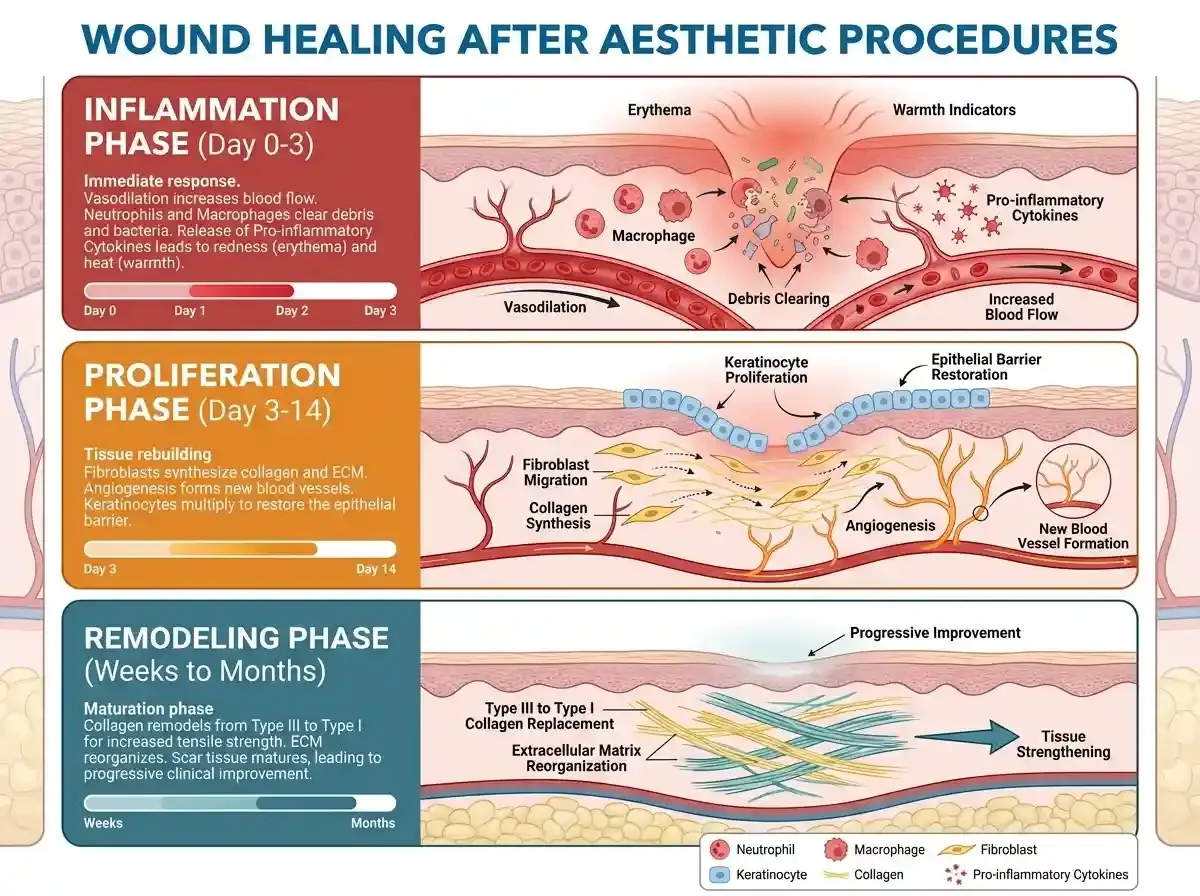
All effective aesthetic procedures, whether microneedling, laser resurfacing, chemical peels, or RF treatments, work by creating controlled injury that triggers the body's regenerative response. This response unfolds in three overlapping phases, each with distinct characteristics and care requirements.
The inflammatory phase begins immediately and typically peaks within 24 to 72 hours. Vasodilation increases blood flow to the area (causing erythema and warmth). Neutrophils and macrophages arrive to clear debris and pathogens. Pro-inflammatory cytokines orchestrate the repair response. This inflammation is necessary and beneficial, but if excessive or prolonged, it can lead to complications including post-inflammatory hyperpigmentation, prolonged erythema, or aberrant scarring.
The proliferation phase follows, typically spanning days 3 through 14. Fibroblasts migrate to the wound site and begin synthesizing collagen and extracellular matrix components. Angiogenesis establishes new blood supply. Keratinocytes proliferate to restore the epithelial barrier. During this phase, the skin is actively rebuilding but remains vulnerable due to incomplete barrier function.
The remodeling phase continues for weeks to months. Initial collagen (primarily type III) is replaced with stronger type I collagen. The extracellular matrix is reorganized for optimal structure and function. This is when patients see progressive improvement in texture, firmness, and overall quality, the delayed gratification that makes follow-up appointments so valuable for demonstrating outcomes.
Barrier Function: The Critical Variable
Virtually every aesthetic procedure compromises the stratum corneum, the skin's barrier layer. This barrier normally prevents transepidermal water loss (TEWL) and protects against pathogen entry and irritant penetration.
When barrier function is compromised, TEWL increases significantly, patients experience the tight, dry sensation that characterizes post-procedure skin. Simultaneously, permeability to external substances increases. This enhanced permeability is why topical products absorb more effectively after procedures, but it also means irritants and pathogens pose greater risk.
Research demonstrates that supporting barrier recovery accelerates overall healing. Products containing ceramides, fatty acids, cholesterol, and humectants like hyaluronic acid help restore the lipid matrix that comprises the "mortar" between corneocytes. This restoration reduces TEWL, improves patient comfort, and creates conditions for optimal healing.
Managing Inflammation: The Balance Point
The clinical challenge with inflammation is maintaining the balance between necessary healing signals and excessive inflammatory response that causes complications.
Anti-inflammatory ingredients can reduce patient discomfort and visible erythema without completely suppressing the healing response. Key agents include niacinamide, which has demonstrated anti-inflammatory properties while supporting barrier function; centella asiatica, whose active compounds (asiaticoside, madecassoside) modulate inflammation while supporting collagen synthesis; panthenol, which calms irritation while supporting barrier repair; and allantoin, which soothes and promotes cell proliferation.
The goal is not to eliminate inflammation but to modulate it, reducing excessive response while preserving the signaling necessary for regeneration.
Protocol Design Principles
Effective aftercare protocols share certain characteristics regardless of the specific procedure. These principles should guide protocol development for your practice.
Phase-Appropriate Care
What the skin needs on day one differs from what it needs on day seven. Protocols should recognize the distinct phases of healing and adjust recommendations accordingly.
During the acute phase (typically days 0 to 3), priorities include protecting compromised skin from infection and irritation, providing hydration to compensate for increased TEWL, calming acute inflammation without suppressing healing, and avoiding any potentially irritating ingredients or activities.
During the repair phase (typically days 4 to 14), priorities shift to continuing barrier support while the lipid matrix rebuilds, introducing ingredients that actively support regeneration, gradually normalizing the skincare routine as tolerance allows, and maintaining rigorous sun protection.
During the optimization phase (week 3 and beyond), patients can resume active ingredients as appropriate for their skin goals, utilize the enhanced receptivity of newly resurfaced skin, focus on maintaining and enhancing results, and continue protective measures especially sun avoidance.
Clear, Actionable Instructions
Patients retain a fraction of verbal instructions. Written protocols that specify exactly what to do, when to do it, and what to avoid dramatically improve compliance. The most effective protocols include day-by-day timelines, specific product recommendations (not just categories), clear lists of what to avoid, visual aids where helpful, and information about what's normal versus what warrants a call.
Many practices find that providing a "kit" with appropriate products ensures patients have what they need and eliminates the guesswork of product selection.
Procedure-Specific Modifications
While general principles apply broadly, specific procedures require tailored protocols.
Microneedling protocols should account for the open channels that persist for several hours post-procedure, enhanced product absorption during this window, typically faster recovery than ablative procedures, and specific guidance on when to resume makeup and exercise.
Laser protocols vary dramatically based on ablative versus non-ablative treatment and fractional versus full-field approaches. Ablative treatments may require wound care approaches (ointment-based healing) before transitioning to standard moisturization. Non-ablative treatments typically require less intensive intervention.
Chemical peel protocols should address the peeling process itself, specifically, the importance of not manually exfoliating peeling skin. Depth of peel determines recovery timeline and protocol intensity.
RF and combination treatments that include thermal injury may have additional considerations regarding heat avoidance and managing any grid-pattern marking.
Managing Patient Expectations
A significant portion of post-procedure dissatisfaction stems not from complications but from unmet expectations. Patients who don't know what to expect interpret normal healing events as problems.
Effective protocols include anticipatory guidance. They explain that redness is normal and expected for a specific duration, that peeling or flaking may occur in a particular timeframe, that results develop over a specified period, that certain activities must be avoided and for how long, and what signs warrant contacting the office versus what is normal.
This anticipatory guidance reduces anxiety, reduces callbacks, and helps patients evaluate their recovery accurately.
Advanced Technologies in Post-Procedure Care
Post-procedure skincare has evolved beyond basic moisturization. Advanced ingredient technologies can actively support and potentially accelerate healing.
Growth Factors and Peptides
Growth factors are signaling proteins that regulate cellular processes including proliferation, migration, and differentiation. In the context of wound healing, they orchestrate the repair response.
Epidermal Growth Factor (EGF) stimulates keratinocyte proliferation and migration, supporting epithelial restoration. Transforming Growth Factor Beta (TGF-β) promotes fibroblast activity and collagen synthesis. Various peptides mimic growth factor activity or support extracellular matrix production.
Clinical studies demonstrate that growth factor-containing products can accelerate re-epithelialization and improve outcomes when applied to post-procedure skin. Their use is particularly compelling given the enhanced penetration that occurs through compromised barrier.
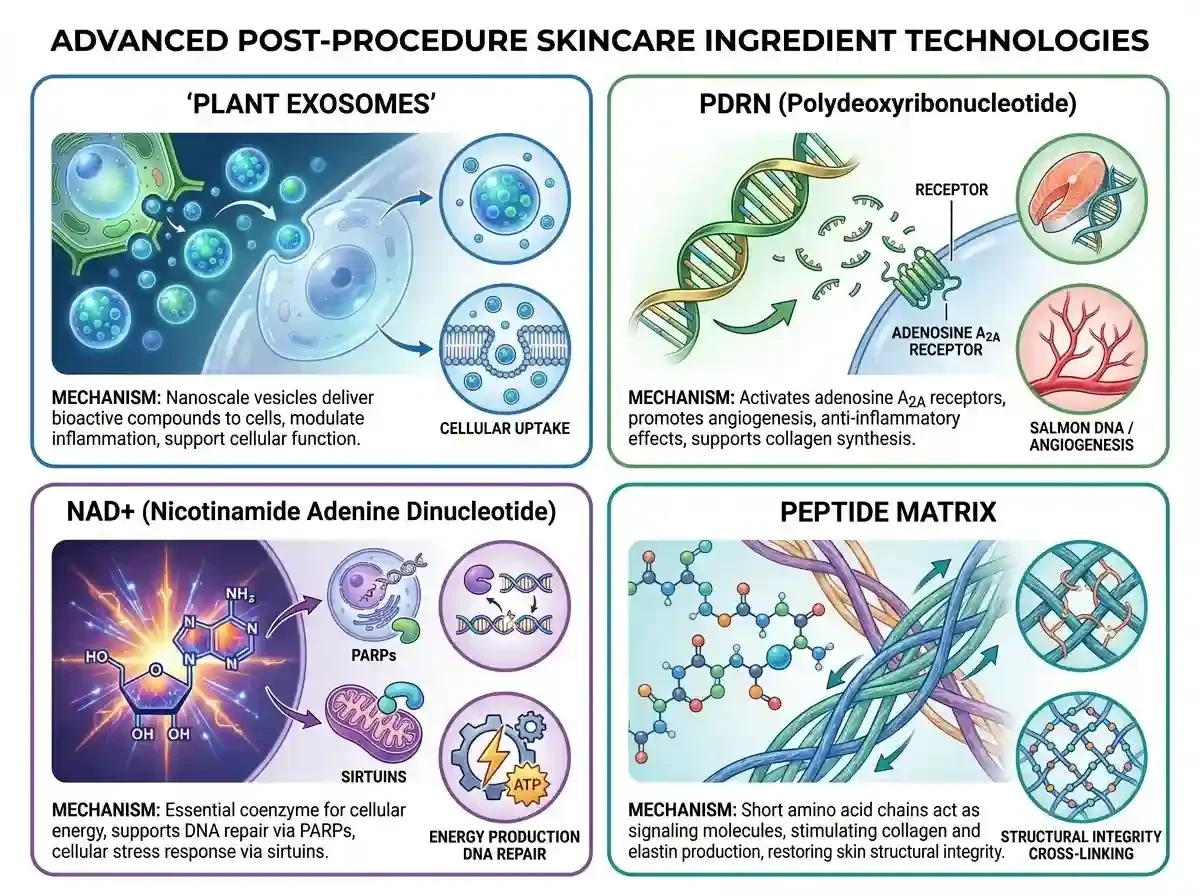
PDRN (Polydeoxyribonucleotide)
PDRN, derived from salmon DNA, represents a sophisticated approach to supporting tissue repair. Its mechanism involves activation of adenosine A2A receptors, which triggers downstream signaling cascades including the cAMP → PKA → VEGF pathway.
This activation promotes angiogenesis (supporting nutrient delivery to healing tissue), has anti-inflammatory effects, and supports fibroblast activity and collagen synthesis. PDRN has been used in wound healing and regenerative medicine contexts before being adopted by aesthetic medicine.
For post-procedure applications, PDRN offers the potential to support the body's natural repair mechanisms at the molecular level, potentially accelerating recovery while supporting optimal collagen production.
Plant Exosomes
Exosomes are nanoscale extracellular vesicles that cells use for intercellular communication. They carry cargo including proteins, lipids, and nucleic acids that can influence recipient cell behavior.
Plant-derived exosomes, particularly those from sources like centella asiatica and panax ginseng, can deliver bioactive compounds directly to skin cells. Their lipid bilayer structure facilitates cellular uptake, while their cargo can modulate inflammatory responses and support cellular function.
In post-procedure applications, plant exosomes represent a delivery mechanism that can enhance the efficacy of bioactive ingredients while potentially providing direct benefits through their inherent cargo.
NAD+ (Nicotinamide Adenine Dinucleotide)
NAD+ is a coenzyme essential for cellular metabolism, serving as a critical cofactor in ATP production. Beyond energy metabolism, NAD+ is a rate-limiting substrate for enzymes including PARPs (involved in DNA repair) and sirtuins (involved in cellular stress response and longevity pathways).
Healing skin has increased energy demands. Supporting NAD+ availability may help cells meet these demands while maintaining genomic stability and optimal function during the repair process.
Topical NAD+ formulations are emerging as a way to support cellular function during the demanding post-procedure period, complementing other active ingredients that address barrier function and inflammation.
The Synergistic Approach
While individual active ingredients offer benefits, the complexity of post-procedure recovery suggests that multi-modal approaches may be optimal. Barrier compromise, inflammation, cellular energy demands, and tissue rebuilding occur simultaneously. Addressing multiple aspects of recovery with complementary ingredients creates a more comprehensive support system than any single ingredient can provide.
This is the rationale behind formulations that combine multiple advanced technologies, creating synergy that addresses the full spectrum of post-procedure skin needs.
Implementation: Integrating Advanced Aftercare into Practice
Translating protocol knowledge into practice implementation requires attention to workflow, staff training, patient communication, and product selection.
Developing Your Protocol Library
Create written protocols for each procedure type you offer. These protocols should be specific enough to guide patient behavior while allowing for clinical judgment in individual cases. Include day-by-day instructions for the acute phase, product recommendations with specific names (generic categories like "gentle moisturizer" invite poor choices), explicit lists of what to avoid, timeline expectations for recovery milestones, and criteria for contacting the office.
Review and update protocols periodically as new evidence and products become available.
Staff Training and Alignment
Everyone in your practice who interacts with post-procedure patients should understand your protocols and be able to answer common questions consistently. This includes clinical staff who perform or assist with procedures, front desk staff who field phone calls, and anyone who sells or discusses aftercare products.
Consistency in messaging builds patient confidence. Conflicting advice erodes trust and increases anxiety-driven callbacks.
Consider creating quick-reference guides for staff covering common questions and their answers, red flags that require clinical attention, and product recommendations and their rationale.
Patient Education and Handoff
The transition from procedure to at-home recovery is a critical moment. Patients are often still processing the treatment experience and may not retain detailed verbal instructions.
Best practices include providing written instructions before the patient leaves, walking through key points verbally while referencing the written document, demonstrating product application if providing a kit, confirming the patient has appropriate products at home, scheduling or discussing follow-up, and providing clear guidance on how to reach the practice with questions.
Some practices send follow-up communications (text, email, or app notification) at key points, day 1, day 3, day 7, with relevant reminders and reassurance.
Product Selection and Dispensing
The products you recommend should meet certain criteria. They should be evidence-based, with ingredients supported by clinical research. They should be appropriate for compromised skin, meaning free of common irritants, fragrance, and potentially sensitizing ingredients. They should be convenient enough that patients will actually use them. And they should be differentiated from mass-market alternatives, providing genuine benefit that justifies the recommendation.
Many practices find that providing curated kits simplifies the patient experience and ensures compliance. Patients receive exactly what they need, eliminating the risk of poor product selection and the friction of sourcing products independently.
From a practice economics perspective, aftercare products represent a revenue opportunity that aligns with patient care goals. Patients benefit from optimized products; practices benefit from margin and the practice-building effects of superior outcomes.
Procedure-Specific Protocol Frameworks
The following frameworks provide starting points for procedure-specific protocols. Adapt them based on your specific techniques, patient population, and product offerings.
Microneedling Protocol Framework
Immediately post-procedure while the patient is still in the office, apply a hydrating serum appropriate for open-channel skin. Consider growth factor or advanced formulations given enhanced absorption. Allow absorption before the patient leaves.
Provide the patient with home instructions covering day 0, which includes no washing unless serum was applied, no touching face, sleeping on clean pillowcase with head elevated. Days 1 through 3 should cover gentle cleansing with approved cleanser, post-procedure serum application twice daily, moisturizer application as needed, mineral SPF if any sun exposure, and avoidance of makeup, active ingredients, exercise, and heat. Days 4 through 7 allow continuation of post-procedure products, gradual return to light activity, and makeup resumption if skin is comfortable. Days 8 through 14 allow gradual reintroduction of regular products, continued post-procedure serum use as desired, and continued sun protection.
Tell the patient to expect redness for 1 to 3 days, possible dryness and mild peeling around days 3 to 5, and visible improvement starting around day 7.
Laser Protocols
Ablative Laser Protocol Framework
Immediately post-procedure, apply initial wound care product as per your established protocol. Provide detailed wound care instructions and ensure the patient has necessary supplies.
Home instructions for days 1 through 5 should include cleansing 4 to 6 times daily with saline or diluted vinegar solution, applying prescribed ointment or occlusive healing product, keeping skin moist at all times, avoiding any other products or makeup, avoiding heat, exercise, and sun, and sleeping with head elevated. Days 5 through 10 allow transition to lighter moisturizers as directed, continued gentle cleansing, no picking at crusting or peeling skin, continued sun avoidance, and makeup consideration only once fully re-epithelialized (typically day 10 to 14). Days 10 through 14 and beyond allow post-procedure serum introduction to support collagen production, gradual activity resumption, continued vigilant sun protection, and active ingredient reintroduction around week 6 or as directed.
Tell the patient to expect significant redness for 1 to 2 weeks, possible oozing in the first few days, crusting and peeling as skin heals, and pink color that fades over weeks to months.
Non-Ablative Laser and IPL Protocol Framework
Immediately post-procedure, apply soothing serum or moisturizer. Apply mineral SPF if the patient will have any sun exposure before reaching home.
Home instructions for days 1 through 3 should cover gentle cleansing, hydrating serum application, moisturizer application, mineral SPF 50 for any sun exposure, and avoidance of active ingredients and heat exposure. Days 4 through 7 allow continuation of gentle routine, makeup resumption if desired, gradual activity resumption, and continued sun protection. Day 7 and beyond allow gradual active ingredient reintroduction and continued post-procedure products as desired.
For IPL specifically, tell the patient to expect that treated pigmented spots will darken before flaking off over 7 to 14 days. Emphasize no picking at darkened spots.
Chemical Peel Protocol Framework
Protocols vary significantly based on peel depth. This framework applies to medium-depth peels.
Immediately post-procedure, apply post-peel soothing product as per your protocol. Provide clear instructions about the peeling process.
Home instructions for days 1 through 3 should cover gentle cleansing only if comfortable, frequent moisturizer application to maintain hydration, strict sun avoidance, and avoidance of active ingredients, makeup, and heat. Days 3 through 7 encompass the peak peeling period during which the patient must not pick, pull, or manually exfoliate. Continued frequent moisturization helps manage tightness and discomfort. Sun avoidance remains critical. Days 7 through 14 allow post-procedure serum introduction as peeling resolves, makeup resumption once skin is comfortable, continued sun protection, and gradual active ingredient reintroduction after day 10.
Tell the patient to expect tight, possibly uncomfortable skin in the first few days, visible peeling typically starting around day 3 and lasting several days, and pink new skin that requires protection as it emerges.
Measuring Outcomes and Optimizing Protocols
Effective practices treat aftercare protocols as living documents, subject to continuous improvement based on outcomes data.
Metrics to Track
Post-procedure callback volume measures how many patients call with questions or concerns in the days following treatment. A well-designed protocol should reduce unnecessary callbacks while ensuring patients know when to call for legitimate concerns.
Complication rates track the incidence of prolonged erythema, infection, PIH, or other adverse outcomes. While some complications are unavoidable, consistent patterns may indicate protocol gaps.
Patient satisfaction scores gathered through formal surveys or informal feedback measure how supported patients feel during recovery and how satisfied they are with outcomes.
Product compliance assesses whether patients actually use recommended products. Non-compliance may indicate cost barriers, confusion, or inconvenience that protocol modifications could address.
Repeat treatment and referral rates serve as downstream indicators of patient satisfaction. Satisfied patients return and refer; dissatisfied patients do neither.
Continuous Improvement
Review outcome data periodically and look for patterns. If certain procedures generate more callbacks, examine whether the protocol adequately prepares patients for what to expect. If compliance is low for certain products, explore why, and whether alternatives might work better.
Stay current with emerging evidence and technologies. Post-procedure care is an evolving field, and practices that adopt effective innovations early can differentiate themselves while improving outcomes.
Solicit staff feedback. Those who field patient calls and observe recoveries often have insights into what's working and what isn't.
The Nexovia Approach: Bio-Intelligent Aftercare
Clinical Protocol Integration
Nexovia's protocol is designed for seamless integration into practice workflows.
The Nexovia Protocol for Professional Use
In-Clinic Application (Day 0):
Your team applies 5 mL immediately post-procedure. For microneedling and non-ablative treatments, apply while channels are open or skin is freshly treated. For ablative laser, apply once wound care protocol allows transition from ointment-based care.
Patient Home Care Instructions:
Acute Recovery (Days 1–7):
Dosage: 1 mL morning + 1 mL evening (2 mL daily)
Follow with bland moisturizer and SPF 50
Patients should avoid retinoids, AHAs/BHAs, exfoliation, intense exercise, and heat exposure
This phase delivers maximum benefit from PDRN and plant exosomes when skin is most receptive
Barrier Restoration (Days 8–14):
Dosage: 0.5 mL morning + 0.5 mL evening (1 mL daily)
Continue barrier support with moisturizer and sun protection
NAD+ and peptide matrix support ongoing collagen production beneath the surface
Patients may begin cautiously reintroducing regular products toward end of this phase
Maintenance (Day 15 until next procedure):
Dosage: 0.5 mL daily
Supports continued collagen remodeling (which continues 3–6 months post-procedure)
Provides ongoing anti-aging benefits between treatments
Patients may continue indefinitely for long-term skin health
Protocol Notes:
For ablative laser patients, begin Nexovia once transitioned from ointment-based wound care (typically around day 5–7)
One 30 mL bottle supports one full recovery cycle
Patients often choose to continue Nexovia long-term due to cumulative anti-aging benefits
Practitioner Partnership
Nexovia is committed to supporting practitioners with comprehensive resources for protocol implementation.
Our Practitioner Kit includes procedure-specific protocols with stepwise instructions tailored for distinct modalities, patient Q&A handouts addressing common post-care concerns to reduce callbacks, staff briefing materials for team alignment on dosing and usage, marketing assets for communicating aftercare value to patients, and in-clinic display materials.
We believe aftercare should be an exact science. Our team is currently finalizing clinical evaluations to certify the Skin Serum's performance in post-procedural recovery and advanced anti-aging capabilities, with standardized endpoints including TEWL, Erythema Index, and skin elasticity measurements.
Nexovia was developed specifically to address the complexity of post-procedure recovery—not as a repurposed daily skincare product, but as a purpose-built solution for compromised, healing skin.
The ABA.4 Bio-Intelligent Architecture
Nexovia's formulation combines four advanced active technologies in one synergistic formula, addressing the multiple simultaneous needs of post-procedure skin.
Plant Exosomes at 4 billion particles per milliliter, derived from Centella Asiatica and Panax Ginseng, deliver bioactive compounds to modulate inflammation and support barrier homeostasis through enhanced cellular communication.
PDRN at 1% concentration (10,000 PPM Sodium DNA) activates adenosine A2A receptor signaling to promote angiogenesis, soft tissue repair, and de novo collagen synthesis through the cAMP → PKA → VEGF pathway.
NAD+ at 1% concentration (10,000 PPM Nicotinamide Adenine Dinucleotide) supports cellular energy production and DNA repair, serving as a rate-limiting substrate for PARPs and sirtuins involved in cellular repair and longevity pathways.
Peptide Matrix featuring EGF-mimetics and Matrikines signals fibroblasts to reinforce extracellular matrix components, restoring elasticity and structural density while supporting overall tissue repair.
This multi-modal approach addresses barrier compromise, inflammation, cellular energy demands, and tissue rebuilding simultaneously, the comprehensive support that post-procedure skin requires.
Preliminary results from ongoing clinical evaluation. Full study data with standardized efficacy endpoints expected April 2026.
Advanced Aftercare for Superior Results
Elevate your practice's aftercare standard with bio-intelligent post-procedure solutions.
Nexovia's Skin Serum was formulated specifically for professional aesthetic settings. The ABA.4 Bio-Intelligent Architecture combines four synergistic technologies, plant exosomes at 4 billion particles per milliliter, PDRN at 1%, NAD+ at 1%, and a peptide matrix to support optimal patient outcomes.
For wholesale inquiries and practitioner partnerships:
Email: hello@nexovia.pro
Phone: +1 307-400-7006
Frequently Asked Questions
-
Standardized aftercare ensures patients receive evidence-based care throughout recovery, reducing variability that leads to complications or suboptimal results. Protocols that support barrier function, modulate inflammation, and provide active regeneration support create optimal conditions for healing. Studies demonstrate that patients receiving structured post-procedure care experience faster recovery, fewer complications, and higher satisfaction with outcomes compared to those receiving generic or inconsistent guidance.
-
PDRN has been studied extensively in wound healing and regenerative medicine contexts, with demonstrated mechanisms including A2A receptor activation, VEGF upregulation, and anti-inflammatory effects. Plant exosomes represent a newer technology with emerging evidence supporting their role in cellular communication and delivery of bioactive compounds. While the aesthetic application of these ingredients is newer than their use in wound healing, the underlying mechanisms are well-characterized and directly relevant to post-procedure recovery.
-
Most callbacks stem from patient anxiety about whether their recovery is normal. Protocols that include anticipatory guidance, clearly explaining what to expect and when, reduce this anxiety by helping patients evaluate their recovery accurately. When patients know that redness lasting three days is expected, they don't call to ask if their redness on day two is concerning. Clear written instructions, specific product recommendations, and defined criteria for when to call further reduce unnecessary contacts while ensuring patients reach out for legitimate concerns.
-
Premium aftercare products can improve outcomes, reduce complications, increase patient satisfaction, and create margin for the practice. Patients who heal faster and better become satisfied patients who return and refer. The cost of the product is typically offset by reduced callback-handling time, fewer complication-management appointments, and increased patient lifetime value. Additionally, practices that offer curated aftercare differentiate themselves in a competitive market.
-
Ablative treatments create open wounds requiring more intensive wound care protocols, often including occlusive ointment-based healing, frequent cleansing, and longer periods avoiding makeup and activity. Non-ablative treatments leave the epidermis intact, requiring less intensive intervention focused on hydration, inflammation modulation, and barrier support. Protocol intensity, duration, and specific product recommendations should scale with treatment invasiveness.
-
General guidelines suggest waiting at least 5 to 7 days after non-ablative treatments and at least 2 weeks after ablative treatments, with some practitioners recommending 6 weeks for full-field ablative resurfacing. However, this varies by treatment intensity and individual healing. The principle is to wait until the barrier is substantially restored and acute inflammation has resolved. Premature reintroduction of actives can cause irritation, prolonged inflammation, and potential complications including PIH.
-
Nexovia is designed for easy protocol integration. For in-clinic application, apply the serum immediately post-procedure during the enhanced-absorption window. For home care, patients use the serum twice daily during the acute phase and continue during the restoration phase. The protocol layers onto your existing cleansing and sun protection recommendations. Our practitioner resources include detailed protocol guides for various procedure types that you can adapt to your specific practice.
-
Yes, Nexovia offers wholesale pricing for aesthetic practices. Contact our professional team at hello@nexovia.pro to discuss partnership opportunities, pricing, and minimum order quantities. We also provide marketing materials and patient education resources to support your aftercare offerings.
This content is intended for aesthetic medicine professionals. Clinical protocols should be adapted based on individual patient factors, specific treatment parameters, and professional judgment. Nexovia is a cosmetic product; claims regarding outcomes are based on ingredient-level research and mechanism of action.